
Cardiovascular disease (CVD) encompasses a range of heart and blood vessel disorders, including coronary artery disease, heart failure, arrhythmias, and stroke. It remains the leading cause of death globally, claiming millions of lives annually. Factors contributing to CVD include hypertension, hyperlipidemia, diabetes, obesity, smoking, and a sedentary lifestyle. Understanding these conditions and their underlying causes is crucial for effective prevention and management.
The mechanisms behind cardiovascular disease often involve atherosclerosis, a process where plaque builds up in the arteries, leading to narrowed and hardened vessels. This condition restricts blood flow and increases the risk of heart attacks and strokes. Moreover, chronic inflammation and oxidative stress play significant roles in the progression of atherosclerosis, further complicating the disease.
Public awareness and education about cardiovascular disease are essential to reduce its prevalence. Early detection through regular health check-ups and monitoring of blood pressure, cholesterol levels, and blood glucose can help identify individuals at risk. By understanding the disease’s multifaceted nature, healthcare professionals can implement more effective strategies to combat CVD.
Exercise physiologists specialise in the study of the body’s responses to physical activity and the role of exercise in health and disease management. Their expertise is invaluable in combating cardiovascular disease, as they design and implement exercise programs tailored to individual needs. These professionals possess a deep understanding of how exercise impacts heart health, making them essential allies in the fight against CVD.
One of the primary responsibilities of exercise physiologists is to assess patients’ physical fitness levels and cardiovascular health. They conduct various tests, such as VO2 max, stress tests, and body composition analysis, to gather comprehensive data. This information is crucial for developing personalised exercise plans that address specific health concerns and limitations.
Moreover, exercise physiologists educate patients about the importance of physical activity and guide them on incorporating exercise into their daily routines. They empower individuals to take control of their health by fostering a proactive approach to preventing and managing cardiovascular disease through regular physical activity.
Engaging in regular physical activity offers numerous benefits for cardiovascular health. Exercise helps reduce the risk of developing heart disease by improving blood circulation, lowering blood pressure, and enhancing the overall function of the cardiovascular system. It also aids in weight management, which is crucial for preventing obesity—a significant risk factor for CVD.
Aerobic exercises, such as walking, running, swimming, and cycling, are particularly effective in promoting heart health. These activities increase the heart rate, improve lung capacity, and enhance the body’s ability to utilise oxygen. Regular aerobic exercise strengthens the heart muscle, enabling it to pump blood more efficiently and reducing the risk of heart disease.
Additionally, resistance training, such as weightlifting, also contributes to cardiovascular health by improving muscle strength and endurance. This type of exercise helps maintain healthy blood sugar levels, reduces inflammation, and improves cholesterol profiles. Combining aerobic and resistance training provides a well-rounded approach to cardiovascular fitness, ensuring comprehensive benefits.
Accurate assessment of cardiovascular risk factors is essential for developing effective exercise programs. Exercise physiologists begin by conducting thorough evaluations of patients’ medical histories, lifestyle habits, and current fitness levels. This comprehensive assessment helps identify individuals at high risk for cardiovascular disease and tailor interventions accordingly.
Key risk factors that exercise physiologists consider include hypertension, high cholesterol levels, diabetes, smoking, obesity, and a sedentary lifestyle. They also evaluate family history, age, gender, and other non-modifiable factors that may contribute to cardiovascular risk. By understanding these risk factors, exercise physiologists can design personalised exercise programs that address specific health concerns.
In addition to traditional risk factors, exercise physiologists may also assess patients’ psychological well-being and stress levels. Chronic stress and mental health issues can significantly impact cardiovascular health, making it essential to address these factors in a holistic approach to disease prevention and management.
Creating individualised exercise programs is a cornerstone of exercise physiology. Exercise physiologists use the data gathered from assessments to design personalised plans that cater to each patient’s unique needs and goals. These programs typically include a combination of aerobic, resistance, and flexibility exercises to ensure a comprehensive approach to cardiovascular health.
For patients with cardiovascular disease, exercise physiologists start with low to moderate-intensity exercises, gradually increasing intensity as fitness levels improve. This progressive approach ensures that patients can safely and effectively build their endurance and strength without overexerting themselves. The plans are regularly reviewed and adjusted based on patients’ progress and feedback.
Moreover, exercise physiologists consider patients’ preferences and lifestyle factors when designing exercise programs. They aim to make physical activity enjoyable and sustainable, encouraging long-term adherence. By incorporating activities that patients enjoy, such as dancing, hiking, or playing sports, exercise physiologists enhance motivation and promote lasting lifestyle changes.
Continuous monitoring and evaluation are essential components of effective exercise programs. Exercise physiologists regularly track patients’ progress through follow-up assessments, fitness tests, and patient feedback. This ongoing monitoring helps identify any challenges or barriers that may hinder progress and allows for timely adjustments to the exercise plan.
Exercise physiologists use various tools and technologies to monitor patients’ progress, including heart rate monitors, pedometers, and fitness apps. These tools provide valuable data on exercise intensity, duration, and frequency, helping physiologists make informed decisions about necessary modifications. Regular check-ins with patients also foster accountability and support.
When adjustments are needed, exercise physiologists modify the exercise program to address any emerging issues or changing health status. They may alter the intensity, duration, or type of exercise to ensure continued progress and safety. This dynamic and responsive approach ensures that exercise programs remain effective and aligned with patients’ evolving needs.
Real-life success stories highlight the profound impact of exercise physiology on cardiovascular health. Consider the case of John, a 55-year-old man diagnosed with coronary artery disease. Under the guidance of an exercise physiologist, John embarked on a personalised exercise program that included walking, cycling, and strength training. Over six months, his cardiovascular fitness improved significantly, his blood pressure normalised, and he lost 20 pounds. John’s quality of life improved, and he reported feeling more energetic and confident in managing his condition.
Another inspiring story is that of Maria, a 62-year-old woman recovering from a heart attack. Her exercise physiologist designed a gentle, progressive exercise plan that started with low-intensity walking and gradually incorporated more challenging activities. Maria’s commitment to her exercise program, coupled with lifestyle modifications, resulted in improved heart function, reduced stress levels, and a renewed sense of well-being.
These success stories underscore the transformative power of exercise in managing cardiovascular disease. They demonstrate how personalised exercise programs, coupled with professional guidance and support, can lead to significant improvements in cardiovascular health and overall quality of life.
While exercise plays a crucial role in combating cardiovascular disease, it is only one piece of the puzzle. Lifestyle modifications, such as adopting a heart-healthy diet, quitting smoking, managing stress, and getting adequate sleep, are equally important. Exercise physiologists emphasise the importance of these holistic changes in conjunction with regular physical activity.
A heart-healthy diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can significantly reduce the risk of cardiovascular disease. Exercise physiologists work closely with dietitians and nutritionists to provide patients with dietary guidance that complements their exercise programs. This collaborative approach ensures comprehensive care and optimal outcomes.
Moreover, addressing stress and mental health is vital for cardiovascular health. Chronic stress can lead to hypertension and other cardiovascular issues, making stress management techniques, such as mindfulness, meditation, and relaxation exercises, essential components of a heart-healthy lifestyle. Exercise physiologists educate patients on these practices and integrate them into their overall wellness plans.
Exercise physiologists do not work in isolation; they collaborate with a multidisciplinary team of healthcare professionals to provide comprehensive care for patients with cardiovascular disease. This team often includes cardiologists, primary care physicians, dietitians, physical therapists, and mental health professionals. By working together, they ensure that patients receive holistic and coordinated care.
Effective communication and collaboration among healthcare providers are essential for optimising patient outcomes. Exercise physiologists share their assessments, exercise plans, and progress reports with other team members, ensuring that everyone is informed and aligned in their approach. This collaborative effort enhances the overall quality of care and supports patients in achieving their health goals.
Additionally, exercise physiologists advocate for patients’ needs and preferences within the healthcare team. They act as liaisons, facilitating discussions about exercise and lifestyle modifications and ensuring that patients’ voices are heard. This patient-centred approach fosters trust and empowers individuals to take an active role in their cardiovascular health.
The field of exercise physiology holds immense potential for advancing cardiovascular care. As our understanding of the intricate relationship between exercise and heart health continues to grow, exercise physiologists will play an increasingly vital role in preventing and managing cardiovascular disease. Their expertise in designing personalised exercise programs and promoting lifestyle modifications is indispensable in the fight against CVD.
Looking ahead, advancements in technology and research will further enhance the capabilities of exercise physiologists. Innovations such as wearable fitness devices, telehealth platforms, and artificial intelligence can provide more precise data and personalised insights, enabling exercise physiologists to optimise their interventions. These tools will facilitate remote monitoring, real-time feedback, and adaptive exercise plans, making cardiovascular care more accessible and effective.
Ultimately, the future of exercise physiology in cardiovascular care is bright, with the potential to transform the lives of individuals at risk for or living with cardiovascular disease. By continuing to prioritise patient-centred care, fostering interdisciplinary collaboration, and embracing technological advancements, exercise physiologists will remain at the forefront of cardiovascular health, driving improvements in prevention, management, and overall well-being.
Hey Activ8 Community,
This blog will explore the extremely common condition known as osteoarthritis (OA). To put it into context, worldwide, 500 million people are affected by OA, and it becomes more common as you age. So, settle in as we unpack what osteoarthritis is, who’s most at risk, and the signs to look out for. We’ll also explore simple and practical ways to manage the niggles and stay active, so you can keep doing the things you love. Whether you’re living with OA or supporting someone who is, this post offers helpful info to better understand and manage the condition. Happy reading!


Osteoarthritis happens when the protective cartilage cushioning your joints gradually wears down, leading to pain, stiffness, and reduced movement. It’s most common as we age, but can also develop due to previous joint injuries, repetitive joint use, excess weight and genetics. While anyone can get OA, understanding your risk factors helps you take early steps to protect your joints.

Yes absolutely!
Exercise is one of the best ways to manage OA symptoms. Low-impact activities like walking, swimming, or cycling help lubricate joints without causing extra strain. Resistance exercises that build muscle around affected joints improve stability and reduce pain. Balance and stretching exercises support joint control and flexibility. It’s important to start slowly and only do what can be tolerated, avoid movements that cause pain, and consider personalised guidance from an exercise physiologist for the safest and most effective program.

There are several ways to ease OA pain and stiffness. Regular, gentle exercise helps keep your joints moving and strengthens the muscles that support them. Applying heat or cold packs can soothe aching joints and reduce inflammation. Maintaining a healthy weight also lessens the load on your joints, which can ease discomfort. Over-the-counter pain relief may be useful during flare-ups, and using joint supports or braces can provide extra stability. It’s important to find a balance between activity and rest and to listen to your body’s signals.
Osteoarthritis is the most common type of arthritis and is often described as a “wear and tear” condition. But it’s a bit more complex than that. OA occurs when the protective cartilage that cushions the ends of your bones gradually breaks down, which can eventually lead to bone-on-bone contact. This can cause pain, stiffness, swelling, and reduced movement in the affected joints. It most commonly affects the knees, hips, hands, and spine, but it can occur in any joint. As the cartilage wears away, the bones may start to rub against each other, leading to discomfort and limiting your ability to move the joint freely.
Osteoarthritis is typically diagnosed based on your symptoms and a physical examination by your GP or another healthcare professional. They’ll look for signs such as joint pain, stiffness, swelling, and reduced movement. An X-ray may be used to confirm the diagnosis by showing changes in the joint, like cartilage loss or bone spurs. In some cases, blood tests may be done to rule out other types of arthritis.
While OA is the most common form, there are many other types — including rheumatoid arthritis, psoriatic arthritis, and gout — which have different causes, symptoms, and treatment approaches. That’s why getting the right diagnosis is important for guiding the most effective care.
So, you may be wondering the point at who’s most at risk? Well, transparently, anyone can develop OA, but some people are more likely to be affected than others. Risk factors include:
While OA can’t be cured, understanding who it affects and how it develops is the first step to managing it well and staying active.
Osteoarthritis symptoms often start mild and build up slowly over time. Many people brush them off at first, thinking it’s just part of getting older, but recognising the signs early can make a big difference.
The most common symptoms include:
OA tends to develop gradually. At first, you might only notice occasional discomfort. Over time, the pain can become more persistent and start to interfere with everyday activities, like walking, getting up from a chair, or gripping objects. Some people experience flare-ups where symptoms get worse for a period, then settle down again. Others may find that the condition steadily progresses. Everyone’s experience is different, but being aware of the signs means you can take steps early to manage it and slow it down.
While there’s currently no cure for osteoarthritis, the good news is that there are plenty of ways to manage the symptoms and stay active. With the right approach, many people are able to reduce their pain, improve joint function, and maintain a good quality of life.
Here are some of the most effective strategies:
The goal isn’t to stop moving, but to move smarter, more often. Staying on top of your symptoms and making a few simple lifestyle tweaks can go a long way in helping you keep doing the things you enjoy.

Exercise physiologists play a vital role in helping people with osteoarthritis stay active and manage their symptoms. With a strong understanding of anatomy and how specific conditions impact the body, we can design personalised exercise programs that strengthen the muscles supporting your joints, improve flexibility, and help reduce pain and stiffness. That said, we know one-on-one guidance isn’t for everyone, so let’s chat about what you can start doing in your sessions to support your joints and keep moving well!
A variety of exercise modalities and joint-specific movements play a key role in managing osteoarthritis. Equally important is revisiting the concept of listening to your body, focusing on movements that feel right and avoiding those that might trigger a flare-up. With that in mind, on flare-up days, switch to gentler activities like hydrotherapy or stretching instead of skipping movement altogether.
Cardiovascularly, starting with low-impact activities is incredibly beneficial. These movements help lubricate the joints, boost circulation, and support overall function without putting too much stress on painful areas. Good options include walking, stationary cycling, and swimming. Even just 10–15 minutes a day can reduce stiffness and improve comfort, to gradually build up to around 30 minutes.
Incorporating resistance-based exercises is important to build strength in the muscles around affected joints. Stronger muscles help reduce joint load and improve stability. You might start with simple bodyweight movements like sit-to-stands, step-ups, or incline push-ups, gradually progressing towards more challenging exercises such as Squats, Deadlifts and Bent-over rows as your strength and confidence improve.
Further balance and proprioception exercises to support joint control and reduce the risk of falls. Try things like single-leg stands (with support nearby if needed) or dynamic tandem walking. These activities also improve body awareness and can make everyday movement feel more stable and secure. Finally, don’t forget to include gentle stretching and mobility work. These exercises help maintain joint range of motion and reduce the feeling of tightness. Move slowly through pain-free ranges and focus on the areas that feel stiff.
Osteoarthritis is a common condition, but it doesn’t have to hold you back. With the right knowledge, early action, and a personalised approach to movement and self-care, you can manage symptoms and maintain a good quality of life. Remember, it’s about moving smarter, listening to your body, and making small, sustainable changes that support your joints day by day. If you’re unsure where to start or need further guidance, please reach out to us and take advantage of a free 15-minute telehealth consultation with our exercise physiologist. Here’s to keeping you moving well and enjoying the things you love for years to come!
Written by Paolo Mitry, an Exercise Physiologist at Activ8 Health Club
Cardiopulmonary fitness, often measured as VO2max, is a crucial marker of overall health and physical performance. VO2max refers to the maximum amount of oxygen your body can utilise during intense exercise. It’s a critical indicator of aerobic endurance and cardiovascular health. Improving VO2max can lead to better sports performance, enhanced energy levels, reduced risk of chronic diseases, and just feeling better, but what is the best way to increase it?
In this blog, we’ll explore scientifically-backed strategies to boost your VO2max and highlight the role of Exercise Physiologists in helping you achieve optimal results.
VO2max stands for “volume of oxygen maximum.” It measures how much oxygen your body can use during maximal exercise. The higher your VO2max is, the more efficiently your heart and lungs work together to supply oxygen to your muscles. It’s a key indicator of aerobic fitness, and improving it can enhance endurance, speed, and overall health whilst reducing morbidity and mortality risk factors.

Cardiovascular health is a topic that gets too little attention. It is crucial to ensure you have good cardiovascular fitness because it affects your everyday life and, as mentioned, plays an important role in reducing the likelihood of further morbidity and mortality risks. Research has shown a strong correlation that those with poor cardiovascular fitness are more likely to develop heart disease, high blood pressure and diabetes. This goes without mentioning the extensive links between risk progression in developing morbidities such as Alzheimer’s disease and cancer, which, as a result, increase the overall risk of mortality.
Holistically and put simply, improving your cardiovascular fitness can help you perform your duties of living more efficiently, exercising more effectively, and therefore, living longer!

VO2max is closely linked to your cardiovascular and respiratory systems. A higher VO2max means your heart pumps more blood per beat, your lungs can take in more oxygen, and your muscles are better at using that oxygen for energy. This is especially important for athletes, but even non-athletes can benefit from a higher VO2max.

Reduced Risk of Heart Disease: Studies show that higher VO2max levels are linked to lower risks of cardiovascular diseases.
Enhanced Performance: Whether you’re an athlete or an everyday individual, a higher VO2max will assist with sustaining prolonged exercise, performing at higher intensities, and even recovering.
Better Weight Management: Efficient oxygen use helps burn more calories, aiding in weight control.
Improved Longevity: Research suggests that people with higher VO2max levels tend to live longer, healthier lives.
a) High-Intensity Interval Training (HIIT)
One of the most effective ways to boost VO2max is through High-Intensity Interval Training (HIIT). This involves short bursts of intense exercise followed by periods of rest or low-intensity exercise. Research shows that HIIT can significantly improve VO2max by challenging both your aerobic and anaerobic systems. A typical HIIT session might include the following; however, it can vary in many ways.
To learn more about HIIT training, stay tuned to our future blogs, where we will explain the ins and outs of this fantastic mode of training!
b) Continuous Endurance Training
Long, steady-state cardio sessions at a moderate intensity can also help improve VO2max. This type of training increases the efficiency of your heart and lungs over time. Examples include:
2. Incorporate Strength Training
While VO2max is primarily associated with cardiovascular exercise, strength training can also play a role. Building muscle improves overall fitness and supports better performance in aerobic activities. Adding strength training 2-3 times per week can complement your cardio efforts.
3. Proper Nutrition and Hydration
Your diet plays a crucial role in supporting your cardiovascular fitness. Adequate carbohydrate intake fuels your workouts, while protein supports muscle recovery. Staying hydrated is equally important, as dehydration can negatively impact your VO2 max during exercise.
Here at Activ8 Health Club, we have active health professionals who can give you all the appropriate information, education, and exercise regimens to help improve your cardiovascular fitness, which, in tandem, will improve your VO2Max. Further explanation below explores this notion!
Improving VO2max isn’t just about working harder; it’s about working smarter, and this is where Exercise Physiologists come in. Through understanding the body’s responses to exercise, Exercise Physiologists can design personalised programs to enhance your VO2max safely and effectively.
Benefits of Working with an Exercise Physiologist:
Improving your VO2 max is a journey that requires dedication, consistency, and the right approach. Whether you’re an athlete aiming for peak performance or simply looking to enhance your overall health, incorporating scientifically-backed strategies like HIIT, continuous endurance training, and strength training can make a significant difference. By working with an Exercise Physiologist, you can ensure that your efforts are safe, effective, and personalised to your needs.
Investing in your cardiopulmonary fitness today can lead to a healthier, more energetic future. So, lace up those sneakers, start training, and consider enlisting the expertise of an Exercise Physiologist here at Activ8 Health Club to help you reach your VO2max potential!
If you need further guidance, please reach out to us and take advantage of a free 15-minute telehealth consultation with our exercise physiologist.
Written by Paolo Mitry, an Exercise Physiologist at Activ8 Health Club
Cancer is a word that often comes with fear and uncertainty. However, a growing body of evidence shows that regular exercise can be a powerful tool in both prevention and management. Whether you’re looking to reduce your risk or improve your quality of life during and after treatment, exercise offers numerous benefits. In this blog, we’ll explore how physical activity impacts health and why working with an Exercise Physiologist can make a significant difference in your journey.

Research shows that regular exercise reduces the risk of various diseases, including breast, colon, endometrial, and prostate cancer. Cancer Council Australia recommends at least 150 minutes of moderate-intensity or 75 minutes of vigorous-intensity exercise weekly for prevention. Additionally, recent studies emphasise the importance of exercise during and after treatment, revealing even more benefits.
Each exercise modality offers unique benefits, so a holistic approach can greatly enhance physical and mental well-being in prevention and management. This blog will explore this concept in more depth.
Hormonal Balance and Weight Management
Maintaining a healthy weight is crucial for cancer prevention, as obesity is a known risk factor for various forms of cancer, such as breast, colorectal, and pancreatic cancer. Regular exercise is key to controlling weight by burning calories and building muscle mass, which helps keep body fat in check.
Exercise boosts your metabolic rate, allowing your body to burn excess fat even while at rest. Resistance training is particularly effective because it stimulates muscle growth and enhances glucose uptake. This improvement in insulin sensitivity helps regulate blood sugar levels and reduces estrogen production, which is linked to an increased risk of cancers like breast cancer.
In addition to resistance training, cardiovascular (or aerobic) exercise further supports prevention. Cardiovascular activities help reduce inflammation and boost immune function. An improved immune system is better at identifying and destroying cancer cells, enhancing its ability to detect and fight abnormal cells. Since inflammation is a significant risk factor for many types, reducing inflammation lowers the risk of cancer development.
By combining resistance and aerobic exercises, you achieve better weight management through fat loss and muscle gain, and you also benefit from reduced levels of hormones and growth factors associated with cancer. Exercise regulates important hormones like insulin and estrogen; for instance, high estrogen levels are associated with a higher risk of breast cancer. By burning fat and improving insulin sensitivity, exercise helps lower estrogen levels naturally.
In summary, incorporating both resistance and cardiovascular training into your routine supports overall health and helps reduce risk factors by managing weight, regulating hormones, and enhancing metabolic and immune function.
For those undergoing treatment, exercise might seem like the last thing you want to do. However, staying active can help manage many of the side effects of treatments like chemotherapy and radiation. When exercise is guided and kept within appropriate intensities, it can offer significant benefits. This is where guidance from an Exercise Physiologist becomes invaluable, helping to maximise benefits such as:
Cancer-related fatigue is one of the most common and debilitating side effects of treatment. Surprisingly, regular physical activity can help reduce this fatigue. Studies show moderate exercise, such as walking or swimming, can boost energy levels and improve overall well-being. This exercise modality helps increase stamina and endurance, reducing the overall feeling of fatigue as it enhances cardiovascular fitness, which combats the exhaustion often associated with cancer treatments. Additionally, low-impact activities such as cycling are gentle exercises that promote relaxation, improve energy levels, and help manage fatigue without overexertion.
Any medical diagnosis can take a toll on your mental health, leading to anxiety, depression, and stress. Exercise has been shown to improve mood by releasing endorphins, the body’s natural “feel-good” chemicals. It also provides a sense of normalcy and control during a challenging time. Additionally, participating in group activities fosters social interaction, combating feelings of isolation and improving overall mental well-being, a big thing at Activ8, we pride ourselves on – a good community.
Cancer treatments can lead to muscle loss and decreased mobility. Incorporating strength training and flexibility exercises can help maintain muscle mass and improve range of motion, making daily activities easier and more comfortable. Resistance training strengthens muscles, helping to counteract the muscle loss that can occur during cancer treatment, whilst flexibility exercises improve joint range of motion and prevent stiffness, which is crucial for maintaining mobility and functional independence.
Exercise can also aid in recovery post-treatment by speeding up the healing process and improving cardiovascular health. Staying active helps you regain strength and stamina, allowing you to return to your normal routine faster.
While exercise is beneficial for cancer prevention and treatment, it’s crucial to approach it with caution, especially during treatment. Building on the previous point, the expertise that Exercise Physiologists offer is indispensable. These health professionals specialise in designing safe and effective exercise programs tailored to the needs of individuals with cancer.
Benefits of Working with an Exercise Physiologist:
We hope that this blog has explained the complex nature of exercising and the benefits it has to cancer, but most importantly:
Exercise as a Lifelong Commitment
It’s important to remember that exercise isn’t just a temporary fix during treatment—it should be a lifelong commitment. Staying active after treatment can help prevent recurrence and improve long-term survival rates. It also continues to offer the same benefits of weight management, hormonal balance, and reduced inflammation, all of which contribute to overall health and well-being.
Exercise is a powerful ally in the fight against diseases, offering prevention, treatment, and recovery benefits. By incorporating regular physical activity into your life, you can take control of your health and improve your quality of life at every stage of your journey. Working with an Exercise Physiologist ensures that your exercise regimen is safe, effective, and tailored to your unique needs.
Whether you’re looking to lower your risk or enhance your recovery, remember that exercise is more than just a workout—it’s a vital part of your health and wellness. Start moving today, and take one step closer to a healthier, stronger you.
If you need further guidance, please contact us and take advantage of a free 15-minute telehealth consultation with our exercise physiologist.
Written by Paolo Mitry, an Exercise Physiologist at Activ8 Health Club
Hey there, Activ8 community!
This blog will delve into bone-related conditions known as osteopenia and osteoporosis (OP). These conditions become more prominent as we age; however, we can minimise the risk and impact these have on our lives from an early stage and as we age.
In Australia, among women over 50, 30% have osteopenia, and 15% have osteoporosis, with 20% of men having osteopenia and only 3% having osteoporosis. This difference is largely due to the rapid decrease in estrogen levels in older women. Either way, if you’ve recently been diagnosed with osteopenia or osteoporosis (OP), we want you to know you’re not alone, and there’s a lot that can be done to manage and improve your bone health. Let’s dive into these conditions and how we can help you stay strong and active.
Before delving deep into this, let’s break down the meaning of these words:
Put simply, osteopenia and osteoporosis are conditions that relate to your bones, where they become weaker due to a loss of overall integrity and mineral density. As a result, they are more prone to fractures. Osteopenia is the early stage of Osteoporosis, where bone density is lower than normal but not low enough to be classified as osteoporosis. If left unchecked, osteopenia can progress to osteoporosis, a more severe condition where bones become extremely fragile, significantly increasing the risk of fractures and other bone injuries. A great visual depiction of this can be seen below.
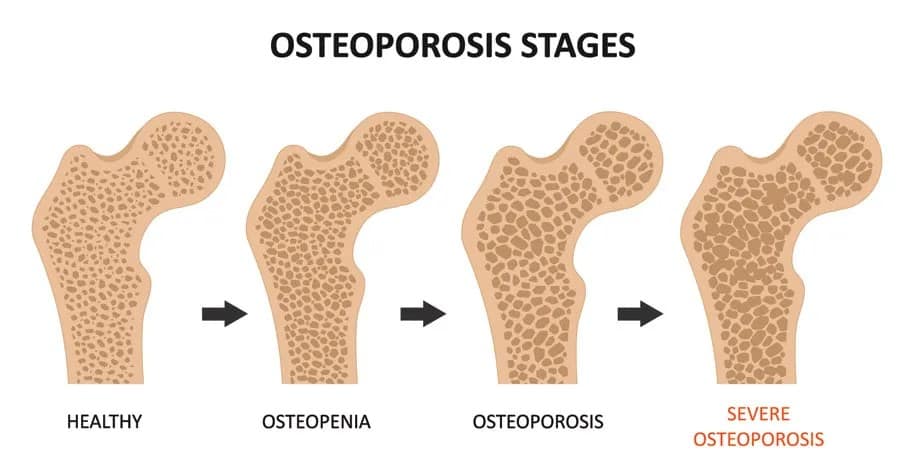
Receiving a diagnosis of osteopenia or osteoporosis is performed through a Dual-Energy X-ray Absorptiometry Scan (DEXA or DXA), and can be determined via a T-score. Below summarises the categories of each score:
These scores are used by healthcare providers to assess bone health and determine the risk of fractures and the need for treatment, which can then help further integrate self-management strategies to aid in this. Diagnosis of either osteoporosis or osteopenia can be a bit of a shock, but it’s important to remember that this isn’t the end of the road. With the right approach, you can manage your condition effectively.
Several factors can contribute to the development of osteopenia and osteoporosis, including:
BUT MOST IMPORTANTLY:
Weight-Bearing Exercises:
Engaging in weight-bearing activities such as resistance training is essential for bone health. These exercises place stress on the bones, stimulating bone formation and helping to maintain or even increase bone density. Resistance training targets specific muscle groups and thus bones, providing resistance that encourages bone growth and strengthening.
Regular participation in these activities helps reduce the risk and treatment of osteoporosis and fractures by maintaining strong, healthy bones. It is never too late to begin resistance exercises for OP. It is critical to know that the higher the force and loads, the greater the growth stimulation will occur, and this must be considered when selecting your exercises. In addition, it is also integral to understand your bones’ safe levels of load to avoid any fractures and progressively overload once they have adapted to the stimulus. It is highly recommended to seek professional advice and guidance when beginning to exercise and treating your OP.
Impact Exercises:
Impact exercises such as jogging and jumping create the greatest mechanical stress on the bones. These stressors stimulate the bone-forming cells (osteoblasts) to increase bone production. The repetitive impact of your feet striking the ground sends signals to your bones to strengthen and rebuild, helping to maintain or even increase bone density. In addition, Impact exercises are particularly effective in slowing down or reversing bone density loss.
Studies have shown that regular participation in weight-bearing activities can lead to significant improvements in bone mineral density, particularly in the hips and spine—areas most vulnerable to osteoporosis-related fractures. It must be noted that these exercises should be gradually introduced into your exercise routine to ensure fractures do not occur
Balance and Flexibility:
Incorporating balance and flexibility exercises into your routine is crucial for overall stability and fall prevention, especially for those with or at risk of osteoporosis. Enhancing your balance can protect against falls, improve joint health, proprioception and your overall confidence. When combined with flexibility training, the risk of falls is significantly reduced, which is particularly important for individuals with weakened bones, as falls are a leading cause of fractures.
At Activ8 Health Club, we believe in empowering you with the knowledge and tools to take control of your health. While some factors are inevitable and irreversible, this section will focus on the positive habits you can adopt to improve your well-being and enhance your quality of life.
With that in mind and to help get you started, we’ve included some of our most beneficial exercises below, along with descriptions to guide you on your journey to better bone health. Whether you’re looking to avoid, reduce, or manage osteopenia or osteoporosis, these exercises can help.
Our exercise physiologists are also here to help design a tailored, safe, and effective program to strengthen your bones and boost your overall health. This approach will cultivate positive habits, support long-term wellness, and optimise your fitness outcomes. Additionally, our vibrant community is filled with supportive and positive individuals. So leap, join us and connect with others on the same journey as you’re not alone!
The leg press is ideal for those with osteoporosis because it strengthens leg muscles and supports bone health by applying controlled resistance, which stimulates bone growth and increases bone density. It’s a safe, low-impact exercise that reduces fracture risk while improving strength and stability, making daily activities easier and safer. Stronger muscles provide better support for your bones, especially in weight-bearing areas like the hips and spine, commonly affected by osteoporosis.
Seated Chest Press
The seated chest press is effective for those with osteoporosis as it builds upper body strength, particularly in the chest, shoulders, and arms. The resistance used in this exercise helps enhance bone density in the upper body. It’s a low-impact, controlled movement that improves overall strength and supports bone health, thereby helping to lower the risk of fractures.
Deadlift
The deadlift is a valuable exercise in combating osteoporosis because it strengthens multiple muscle groups, including the back, glutes, and legs. Lifting weights from the ground supports bone density in the spine and lower body, which are major weight-bearing areas in day-to-day life. This exercise enhances overall strength and stability while being a low-impact option that helps reduce fracture risk.
Assisted Chin-Ups
Assisted chin-ups primarily target the muscles in your upper back, shoulders, and arms, which can help improve overall strength and posture. Stronger muscles around the spine can provide better support and reduce the risk of fractures. Like other resistance exercises, chin-ups provide a stimulus to the bones, particularly in the upper body, which can help maintain or improve bone density in those areas. With this, strengthening the upper body through exercises like assisted chin-ups can improve your ability to perform daily tasks, reducing the likelihood of falls and injuries.
Single Leg Stance
Single-leg stance is a balance exercise that helps combat osteoporosis. It improves stability and strengthens the muscles around the hips and legs. These exercises enhance coordination and support bone health in the lower body by challenging your balance. This simple, low-impact activity helps reduce the risk of falls and fractures by boosting overall balance and strength.
Stepper/Climbmill Machine
Using a stepper/climbmill machine is excellent for osteoporosis because it is a weight-bearing activity that strengthens the legs and hips. Walking/stepping promotes bone health through repetitive impact and offers high engagement to the muscles within the lower body. This, therefore, helps maintain bone density and improve overall stability, reducing the risk of fractures.
Step-Jump Downs
Step jump-downs are beneficial for osteoporosis as they involve jumping down from a height, which strengthens the legs and stimulates bone density through controlled impact. This dynamic movement helps build muscle power and enhances bone health in the lower body. By improving strength and stability, step jump-downs can help reduce the risk of fractures.
What’s The Role of Exercise for OP:

While it may seem counterintuitive to engage in physical activity when dealing with fragile bones, exercise is, in fact, a powerful ally in managing osteopenia and osteoporosis. Here are some key benefits that’ll hopefully encourage you to keep moving!:
1. Strengthening Bones:
Weight-bearing and resistance exercises stimulate bone formation and enhance bone density. Activities like walking, jogging and strength training can put healthy stress on bones, promoting the deposition of minerals and reinforcing their structure.2. Improving Muscle Strength:
Strong muscles act as a protective layer for bones. By engaging in resistance exercises, you not only enhance muscle mass but also provide better support for your skeletal system, reducing the risk of falls and fractures.3. Enhancing Balance and Coordination:
Many individuals with osteoporosis face a higher risk of serious complications from falls. Exercise routines focusing on balance and coordination can help prevent falls and enhance overall stability, reducing the likelihood of such incidents.4. Boosting Joint Flexibility:
Osteoporosis can lead to joint stiffness and discomfort. Regular exercise that includes stretching and flexibility training can alleviate these symptoms, enhancing your range of motion and promoting joint health.5. Maintaining a Healthy Weight:
Excess body weight can strain bones and their relevant joints, thus exacerbating the challenges associated with osteoporosis. Engaging in regular exercise paired with a healthy diet helps manage body weight, therefore reducing the load on bones and joints.6. Enhancing Overall Well-being:
Exercise has numerous benefits beyond bone health. It releases endorphins, the body’s natural mood lifters, which can help combat feelings of anxiety and depression that may accompany a diagnosis of osteopenia or osteoporosis.

Always Check with Your Doctor First
Before starting any exercise program, it’s essential to consult with your healthcare provider. They can offer personalised recommendations based on your specific condition, overall health, and any potential limitations. As highlighted earlier in this blog, participating in various activities can be highly beneficial for combating osteopenia and osteoporosis. Choosing activities you enjoy is key to maintaining adherence to your exercise routine.
Sometimes, the simplest exercise routines can be the most effective, especially when managing conditions like osteoporosis. As mentioned throughout this blog, engaging in low-impact activities helps strengthen bones and joints by targeting the surrounding muscles. It’s important to start at a manageable intensity, allowing your body to adapt gradually. As your body adjusts, the intensity of your workouts should also increase to ensure continued progress and to prevent fractures and injuries. The best part is that these activities can be within a gym environment, and/or an outdoor setting.
The activities you choose must be enjoyable to encourage positive adherence! Don’t feel limited by these recommendations. Hence why, Activ8 Health Club is an excellent choice, as variety and understanding from our exercise physiologists, as well as the positive environment and strong community support, help all individuals on their path to better their lives!
A diagnosis of osteopenia or osteoporosis doesn’t mean a life devoid of physical activity. Exercise is in fact, a vital component of managing these conditions and maintaining a high quality of life. By incorporating weight-bearing exercises, strength training, balance, coordination activities, and flexibility exercises into your routine, you can contribute significantly to the health and resilience of your bones, joints and overall body! Remember, it’s never too late to start, and every step towards a more active lifestyle is a step towards better bone health and overall well-being.
So, if you’ve recently been diagnosed with osteopenia or osteoporosis, don’t worry! You can still engage in numerous physical activity alternatives, but you may require slight alterations! If you follow our recommendations above, we guarantee that you’ll be back to your physically fit lifestyle in no time at all.
If you need further guidance, please reach out to us and take advantage of a free 15-minute telehealth consultation with our exercise physiologist.
Written by Paolo Mitry, an Exercise Physiologist at Activ8 Health Club

Exercise physiologist is a field of study focused on the body’s responses and adaptations to physical activity. This scientific discipline delves into how exercise impacts the cardiovascular, respiratory, metabolic, and musculoskeletal systems. At its core, exercise physiology aims to understand the mechanisms behind exercise-induced improvements in health and performance. This knowledge allows professionals to design effective exercise programs that cater to individual needs and goals.
Working with an Exercise Physiologist can provide you with the tools and strategies necessary to achieve your fitness goals effectively.
The insights from an Exercise Physiologist can help you make informed choices about your exercise regimen.
Regular check-ins with your Exercise Physiologist can keep you motivated and on track.
Working with an Exercise Physiologist allows for tailored strategies to maximise health outcomes.
An Exercise Physiologist can help bridge the gap between fitness and health management.
Understanding the role of an Exercise Physiologist can greatly enhance your fitness journey.
Many individuals benefit from working with an Exercise Physiologist for tailored fitness advice.
Consulting an Exercise Physiologist is essential for anyone serious about improving their health.
Collaborating with an Exercise Physiologist can facilitate significant health improvements.
The origins of exercise physiology can be traced back to ancient civilisations, where physical training was integral to military and athletic success. However, it wasn’t until the 20th century that exercise physiology emerged as a distinct scientific field. Advances in technology and research methodologies have since propelled our understanding of how exercise influences the human body. Today, exercise physiologists use this knowledge to help individuals achieve optimal health and performance.
Exercise Physiologists create plans that reflect individual goals and health conditions.
With the support of an Exercise Physiologist, you can achieve sustainable results.
Exercise physiology encompasses a wide range of topics, including the acute and chronic effects of exercise on the body, the role of physical activity in disease prevention and management, and the impact of different types of exercise on various populations. By studying these areas, exercise physiologists can develop evidence-based strategies to promote health and well-being through physical activity.
Exercise Physiologists use their expertise to create effective health interventions.
Many individuals find success with their fitness plans by working closely with an Exercise Physiologist.
Exercise physiologists are highly trained professionals who specialise in the assessment, prescription, and supervision of exercise programs. They work with clients to improve their physical fitness, manage chronic conditions, and enhance overall well-being. These experts possess a deep understanding of the physiological principles underlying exercise and use this knowledge to create personalised programs that address each client’s unique needs.
One of the primary roles of exercise physiologists is to conduct comprehensive assessments of their clients’ health and fitness levels. This process often involves evaluating factors such as cardiovascular fitness, muscular strength and endurance, flexibility, and body composition. By gathering this information, exercise physiologists can identify areas of improvement and develop tailored exercise plans to help clients achieve their goals.
Each plan crafted by an Exercise Physiologist is unique and tailored to the individual.
In addition to designing and supervising exercise programs, exercise physiologists also provide education and support to help clients adopt and maintain healthy lifestyle habits. This may include guidance on nutrition, stress management, and sleep hygiene, as well as strategies for overcoming barriers to physical activity. By addressing these aspects of health and wellness, exercise physiologists empower clients to make lasting changes that enhance their quality of life.
Benefits of Working with an Exercise Physiologist
Understanding chronic conditions is vital for an Exercise Physiologist when designing programs.
Working with an Exercise Physiologist can lead to better management of health conditions.
Working with an exercise physiologist offers numerous benefits, particularly for individuals with specific health concerns or fitness goals. One of the most significant advantages is the personalised approach that exercise physiologists bring to their work. Unlike generic exercise programs, which may not address individual needs, a tailored plan from an exercise physiologist takes into account each client’s unique circumstances and goals.
Consulting with an Exercise Physiologist can enhance the effectiveness of your fitness journey.
Another key benefit of working with an exercise physiologist is the focus on evidence-based practice. Exercise physiologists rely on scientific research to inform their recommendations and ensure that their clients receive the most effective and safe exercise interventions. This commitment to evidence-based practice helps clients achieve optimal results while minimising the risk of injury or adverse effects.
Additionally, exercise physiologists provide ongoing support and motivation to help clients stay on track with their fitness journeys. Regular check-ins, progress assessments, and adjustments to exercise plans ensure that clients remain engaged and committed to their goals. This level of support can be particularly valuable for individuals who struggle with maintaining a consistent exercise routine or who need additional guidance to overcome obstacles.
Exercise physiologists play a crucial role in the management and treatment of various chronic conditions. These professionals use their expertise to design exercise programs that help clients manage symptoms, improve function, and enhance overall quality of life. Some of the most common conditions treated by exercise physiologists include cardiovascular disease, diabetes, obesity, and musculoskeletal disorders.
Cardiovascular disease is a leading cause of morbidity and mortality worldwide. Exercise physiologists work with individuals who have conditions such as coronary artery disease, heart failure, and hypertension to improve cardiovascular fitness and reduce risk factors. Through carefully designed exercise programs, clients can enhance their heart health, increase their exercise tolerance, and potentially reduce the need for medication.
Diabetes is another condition commonly addressed by exercise physiologists. Regular physical activity plays a vital role in managing blood glucose levels and improving insulin sensitivity. Exercise physiologists create personalised exercise plans that help clients with diabetes achieve better glycemic control, reduce the risk of complications, and enhance overall health. In addition to exercise prescription, they may also provide education on nutrition and lifestyle modifications to support diabetes management.
Creating personalised exercise programs is a cornerstone of the work that exercise physiologists do. This process begins with a thorough assessment of each client’s health status, fitness level, and goals. By gathering detailed information through assessments and consultations, exercise physiologists can develop a comprehensive understanding of the client’s needs and preferences.
The initial assessment typically includes a review of the client’s medical history, current health conditions, and any medications they may be taking. This information is crucial for identifying any potential contraindications or precautions that need to be considered when designing an exercise program. Additionally, exercise physiologists may conduct various fitness tests to evaluate cardiovascular endurance, muscular strength, flexibility, and body composition.
Once the assessment is complete, the exercise physiologist uses the gathered data to create a tailored exercise program. This program is designed to address the client’s specific goals, whether they aim to improve overall fitness, manage a chronic condition, or enhance athletic performance. The exercise physiologist selects appropriate types, intensities, and durations of exercise to ensure the program is both effective and safe. Regular monitoring and adjustments to the program ensure that it continues to meet the client’s evolving needs.
Exercise prescription is an art and a science that involves designing individualised exercise programs based on scientific principles. The goal is to optimise the benefits of physical activity while minimising the risk of injury or adverse effects. Exercise physiologists use a variety of scientific concepts and guidelines to inform their exercise prescriptions, ensuring that clients receive the most effective and safe interventions.
One of the key principles underlying exercise prescription is the FITT principle, which stands for Frequency, Intensity, Time, and Type. Frequency refers to how often exercise sessions are performed, while intensity describes the level of effort required. Time is the duration of each exercise session, and type refers to the specific mode of exercise, such as aerobic, resistance, or flexibility training. By manipulating these variables, exercise physiologists can create a balanced and effective exercise program.
In addition to the FITT principle, exercise physiologists also consider factors such as the client’s age, fitness level, health status, and individual preferences. They use evidence-based guidelines and research to determine the most appropriate exercise interventions for each client. This scientific approach ensures that exercise programs are tailored to meet the unique needs of each individual, maximising the benefits of physical activity while minimising potential risks.
The expertise of an Exercise Physiologist can greatly contribute to your success.
While both exercise physiologists and personal trainers work to improve clients’ fitness and health, there are key differences between these two professions. Understanding these distinctions can help individuals make informed decisions when seeking professional guidance for their exercise and wellness needs.
Exercise physiologists are healthcare professionals with extensive education and training in the science of exercise and its impact on the body. They typically hold advanced degrees in exercise physiology or related fields and are often required to obtain certification from recognised organisations. Their expertise allows them to work with clients who have complex medical conditions, develop evidence-based exercise prescriptions, and collaborate with other healthcare providers to ensure comprehensive care.
Personal trainers, on the other hand, focus primarily on helping clients achieve fitness goals through exercise programming and motivation. While personal trainers may have certifications and training in exercise science, their scope of practice is generally more limited compared to exercise physiologists. Personal trainers often work with healthy individuals or those with less complex health needs, guiding exercise techniques, goal setting, and accountability.
The impact of exercise physiology on individuals’ health and well-being can be profound, as evidenced by numerous success stories. These transformations highlight the power of personalised exercise programs and the expertise of exercise physiologists in helping clients achieve their goals and improve their quality of life.
One inspiring example is that of a middle-aged woman with type 2 diabetes who struggled to manage her blood glucose levels despite medication and dietary changes. After working with an exercise physiologist, she began a tailored exercise program that included aerobic and resistance training. Over time, her blood glucose levels stabilised, her insulin sensitivity improved, and she experienced significant weight loss. With the support of her exercise physiologist, she was able to reduce her reliance on medication and enjoy a more active, fulfilling life.
Another success story involves a man with chronic back pain caused by a herniated disc. Traditional treatments, including physical therapy and pain medication, provided only temporary relief. Seeking a long-term solution, he turned to an exercise physiologist who developed a personalised exercise program focused on strengthening his core muscles and improving his posture. With consistent effort and guidance, his pain diminished, and he regained the ability to participate in activities he once enjoyed.
These stories and many others underscore the transformative potential of exercise physiology. By addressing individual needs and leveraging scientific principles, exercise physiologists help clients overcome challenges, achieve their goals, and lead healthier, more active lives.
Selecting the right exercise physiologist is a crucial step in your health and fitness journey. The right professional will not only have the necessary qualifications and experience but will also be a good fit for your personality and goals. Here are some tips to help you find the right exercise physiologist for you.
First, consider the exercise physiologist’s credentials. Look for professionals who have advanced degrees in exercise physiology or related fields and who are certified by recognised organisations such as Exercise & Sport Science Australia (ESSA). These credentials indicate a high level of expertise and commitment to maintaining professional standards.
Next, evaluate the exercise physiologist’s experience and areas of specialisation. Some exercise physiologists may have specific expertise in working with certain populations, such as older adults, athletes, or individuals with chronic conditions. Finding a professional with experience relevant to your needs can enhance the effectiveness of your exercise program and ensure that you receive the best possible care.
Finally, consider the exercise physiologist’s approach and communication style. A good fit is essential for building a trusting and productive relationship. Schedule a consultation to discuss your goals, ask questions, and gauge whether you feel comfortable with their approach. The right exercise physiologist will listen to your needs, provide clear explanations, and offer support and encouragement throughout your fitness journey.
Embarking on a journey towards better health can be both exciting and challenging. With the guidance and expertise of an exercise physiologist, you can navigate this path with confidence and achieve lasting improvements in your fitness and well-being. These professionals bring a wealth of knowledge and a personalised approach that can make all the difference in reaching your health goals.
Whether you are managing a chronic condition, recovering from an injury, or simply looking to enhance your overall fitness, an exercise physiologist can provide the support and guidance you need. By understanding the science behind exercise and tailoring programs to your unique needs, they help you unlock your full potential and enjoy a healthier, more active life.
Take the first step towards better health by finding a qualified exercise physiologist who can help you achieve your goals. With their expertise and your commitment, you can transform your health journey and unlock a brighter, more vibrant future. Your path to better health starts now—embrace the possibilities and take charge of your well-being today.
If you want to speak with an Accredited Exercise Physiologist (100% free), follow this link and book a free Telehealth consultation. We are here to answer all of your questions.
Written by Trent Carruthers, Accredited Exercise Physiologist at Activ8 Health Club

When it comes to fitness and overall well-being, the term “core muscles” is frequently loosely tossed around. So what exactly are these muscles, and why are they so important to us and our day-to-day living? As we embark on this exploration, let’s uncover the secrets and unravel the vital roles they play in supporting your body.

A major misconception that is thrown around is the consideration of muscles within your “core muscles”. Being able to gain clarity on this will facilitate effective prescription in building a strong core. Comprising all the muscles that act and attach to the spine or pelvis, the three categorised groups involve:
1. Abdominal Muscles – Rectus Abdominus, Internal Obliques, External Obliques & Transverse Abdominus.
2. Posterior/Back Muscles – Thoracolumbar, Lumbar, Lateral Thoracolumbar & Latissimus Dorsi
3. Lower Extremity Groups – Gluteal muscles, Adductor muscles, Hip Rotators, as well as Hamstring & Hip flexor muscles.
Read throughout this blog to delve deeper into the specifics of each considered group and its further muscles!

The role of your core regarding fitness and general health circumstances is critical, rendering these muscles indispensable to the overall makeup and performance of your body. It is not simply labelled the ‘core’ because it is located at the centre of your body; rather, it is a crucial component of our musculoskeletal system that plays a vital role in various movements and functions.
Firstly, appropriate core function aids in stability and posture, particularly within the hips and spine, thereby reducing the likelihood of musculoskeletal imbalances and recurrent pain (particularly lower back pain).
Additionally, being strong in this area facilitates greater movement and flexibility, as well as enhanced balance and coordination. These elements, when working in tandem, allow for greater movement efficiency, effectiveness, and overall performance. Finally, a robust core helps protect internal organs and contributes to an overall healthy balance.

Effective core training involves exercises that target the appropriate muscles collectively, providing strength, stability, and balance to the entire region. As mentioned, your core is made up of numerous muscles and muscle groups that should be worked appropriately through a variety of different exercises.
Trying to keep this as simple as possible to get started, we have split these into our three main groups, with exercises potentially following:
1. Abdominal Muscles: Dead Bug → Russian Twist → Bicycle Crunches
2. Posterior/Back Muscles: Bird Dog → Side Plank → Bent Over Row
3. Lower Extremities: Deadlift → Squat → Bulgarian Split Squat
Following these exercises in a progressive order will help allow for a safe yet effective progression in building the appropriate muscles to create a strong core. Read on and follow future blogs for further information and exercise progressions that can be implemented into your training regimen!
Your core muscles are not just a singular entity but a group of muscles that work together to provide stability, balance, and support to your entire body’s functions. They comprise all the muscles that act and attach to the spine or pelvis. They are primarily within your torso; these also include numerous muscles below your pelvis.
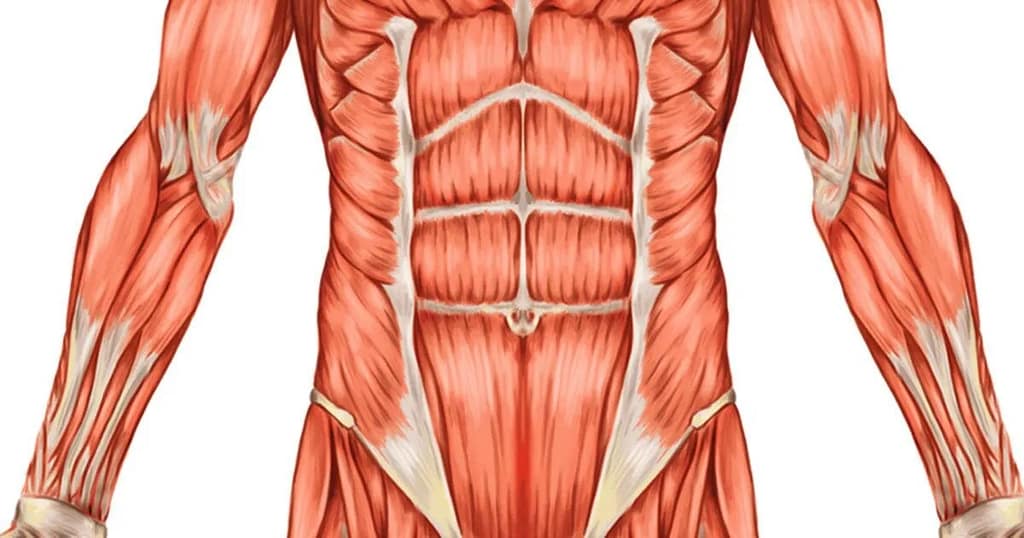
These muscles can be categorised into three (3) main groups:
Now that we’ve identified the key players in your core, let’s delve into the functions that make these muscles indispensable to your body’s overall performance.
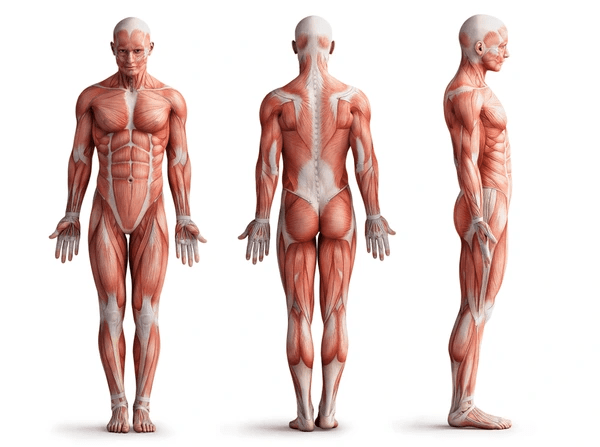
Now that we understand the significance of core muscles, how can we strengthen them? Incorporating targeted exercises into your fitness routine is key. Below are some effective exercises for each group of core muscles, with video demonstrations:
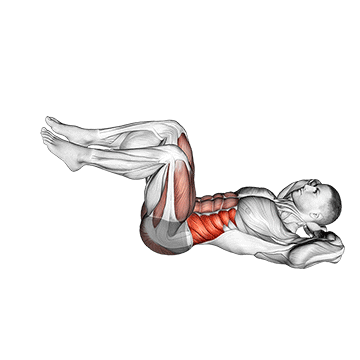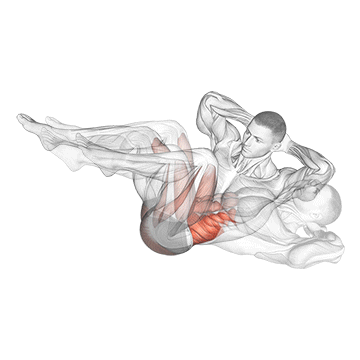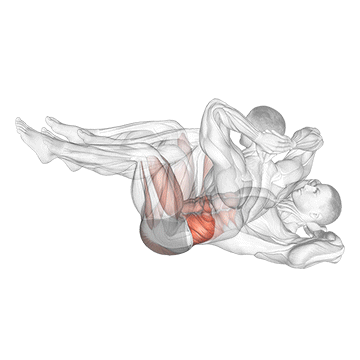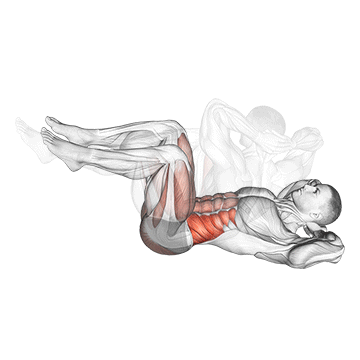
There has been and continues to be a huge body of research regarding the best exercises for increasing core strength. The most recent information indicates that greater recruitment, thus improvements, are achieved via large compound exercises such as squatting and deadlifts. Considering this, it is critical to incorporate these lifts into your routine wherever possible.
Remember to ensure the safety and technique of these exercises before increasing volume and quantity. Further, consider following our future blogs for further information and exercise progressions that can be implemented into your training regime to help continue to build a stronger core session by session!
Your core muscles are the unsung heroes of your body, providing the foundation for strength, stability, and overall well-being. Whether you’re an athlete aiming to improve performance or someone looking to enhance everyday movements, understanding and nurturing your core muscles should be a fundamental part of your fitness journey. So, here’s to a strong and resilient core that supports you in all your endeavours!
If you need further guidance, please reach out to us and take advantage of a free 15-minute telehealth consultation with our exercise physiologist.
Written by Paolo Mitry, an Exercise Physiologist at Activ8 Health Club

The horizontal pull is a key movement pattern that involves moving or pulling a weight towards your chest/torso, and rowing-based movements, such as seated rows and utilising the TRX. The horizontal pull movement is a vital component of strength training that targets the upper back and shoulder muscles. This movement is extremely versatile and can be completed in a variety of ways, allowing for flexibility based on your goals and available resources, offering options for every fitness level and preference.
Incorporating horizontal pull exercises into your routine is key to developing a balanced upper body, improving posture, and enhancing functional strength. Whether you choose free weights, cables, or bodyweight variations, the horizontal pull movement is an essential addition to any well-rounded strength training program. The primary muscles engaged during the horizontal pull involve the latissimus dorsi (lats), rhomboids, trapezius and rear deltoids, as well as your forearm and core muscles.
As with all exercises, it is critical to gradually build up to the more challenging exercises to ensure safety is maintained. Within this blog, you will find some exercise progressions and regressions for you to work through. Additionally, this movement can be further progressed, which will be discussed in future blogs.

Both seated and standing horizontal pulls have various associated benefits, but the choice between the two should align with your goals and any individual considerations you may have. During a seated horizontal pull, you have more stability and isolation of the required muscles to perform the action. Oppositely, standing pulls allow for more variety in movements, as well as greater functional strength benefits due to their ability to mimic movements of our everyday lives. In essence, both seated and standing pulls have great benefits, but training goals, individual considerations, and exercise experience should shape what’s best for you.

Essentially, both single-and double-arm horizontal pulls are extremely beneficial, but their effectiveness is determined by each individual’s training goals and circumstances. It is thought that single-arm pulling is more beneficial due to the isolated targeting of one arm, which can help identify imbalances and reduce discrepancies, as well as hold value in building functional strength. This is due to the necessity of one-hand or arm movements we perform during everyday life. Otherwise, double-arm exercises hold benefits in exercise efficiency due to the ability to shift heavier loads, but prioritising single over double should be determined by your individual goals and personal circumstances.

Absolutely! Utilising the TRX is a great way to perform a horizontal pull movement. Not only does it allow for a wide variety of different exercises, but it serves as a challenge, too. Due to the suspensions not being firmly fixed, activation of surrounding muscles, particularly your core, is required to stabilise yourself as you travel through the movement. Alternatively, the angle at which you situate yourself can make the movement easier or more challenging for you.

During the movement of a horizontal pull, a wide range of exercises can be performed to achieve activation of the required muscle groups. Below is a list of horizontal pull exercises in order of least to most challenging. Within this list, exercise difficulty can continue to vary depending on factors such as the angle at which the movement is performed, as well as the hand grip used. Choosing exercises that match your current fitness level is imperative to progressively challenge yourself whilst ensuring safety is maintained.
1. Seated Row (Double Arm / Single Arm)
2. Standing Cable Row (Double Arm / Single Arm)
3. Double-Arm TRX Row (120°)
4. Bench-Supported Single Arm Dumbbell Row
5. Double-Arm TRX Row (90°)
6. Bent-Over Barbell Row
This movement can be further progressed, which we will discuss in future blogs!
Not only can the horizontal pull movement be made more difficult by changing the type of exercise completed, the weight moved and the range you’re moving through, but also the hand grip you have whilst completing it. This is because it alters the muscles that are primarily engaged. The three main types of hand grips include (from easiest to hardest):
Although the grip utilised may change the difficulty of the exercise, it does not mean the benefits associated with it decline. During a supinated grip, there is greater emphasis on the biceps and less demand on the lats and upper back. With this, there is greater engagement of different muscle groups to help with the movement. For a neutral grip, there is a balance between overhand and underhand grips. This can promote better stability during the movement, allowing for more comfort when being performed. Finally, the pronated grip is most challenging as the range of motion during the movement is generally longer compared to others, whilst only engaging your lats and upper back muscles.
Importantly, the choice of grip should align with your specific goals and training preferences. As you move through your training, utilising different grips and exercises can provide variety and target specific areas of your upper body. Ultimately, the perceived difficulty of an exercise can vary based on factors of strength and experience.
As with all exercises, it is critical that you gradually build up to these more challenging exercises to ensure safety is maintained.
We have provided a safe exercise progression below with video demonstrations of each to help you.
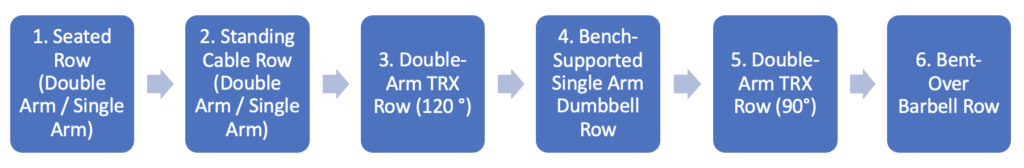
If you have any further questions, please contact us anytime.
NOTE: This exercise can be further progressed, which we will review in further blogs, so stay tuned!
The horizontal pull movement is an extremely fundamental and versatile movement that is critical to add to your training regime. It is a great way to step up your upper body training and achieve some wonderful results.
The Bent-Over Row is a great advanced exercise that should be built up to and introduced once conditioned appropriately. Gradually work towards this by following the progressive exercises explored throughout this blog!
If you need further guidance, please reach out to us and take advantage of a free 15-minute telehealth consultation with our exercise physiologist.
Written by Paolo Mitry, an Exercise Physiologist at Activ8 Health Club

Diabetes is a chronic condition that affects millions of people worldwide. It’s characterised by high blood sugar levels resulting from insulin resistance or insufficient insulin production. While medication and dietary changes are often necessary components of diabetes management, regular exercise has emerged as a powerful and natural ally in the battle against this condition. In this blog, we’ll explore the compelling relationship between regular exercise and the treatment and management of Type II Diabetes.
Diabetes is a chronic condition that affects millions of people worldwide. It’s characterised by high blood sugar levels resulting from insulin resistance or insufficient insulin production. While medication and dietary changes are often necessary components of management, regular exercise has emerged as a powerful and natural ally in the battle against this condition. In this blog, we’ll explore the compelling relationship between regular exercise and treatment.
Regular exercise and Type II Diabetes have a profound connection. Exercise affects blood sugar levels, insulin sensitivity, and overall health in several ways:
Regular exercise offers a multitude of benefits for individuals, including but not limited to the following:
The latest research recommends that those with Diabetes follow the guidelines below:
| Aerobic Exercise | Resistance Exercise | To the point of discomfort | |
| Frequency | 3-7 days/week | Min of 2 non-consecutive / week, preferably 3 days/week | >2-3 days/week |
| Intensity | Moderate (40-60% Vo2 to Vigorous (60-80% Vo2) | To the point of discomfort | To point of discomfort |
| Time | Minimum 150min / week of Moderate to Vigorous Intensity (40-90% Vo2) | 1-3 sets, 10-15 reps for at least 8-10 exercises, training to fatigue | Hold for 10-30sec, 2-4 reps |
| Type | Prolonged, large muscle group exercises | To the point of discomfort | any |
As with any exercise plan, it is important to consider all medical history and your current health circumstances and seek professional guidance when and where possible. Below are some considerations to keep in mind when you are exercising with Diabetes;
Regular exercise helps to lower circulating blood glucose levels. When you exercise, the sensitivity of Insulin within your body increases, increasing your muscle cells’ ability to uptake the glucose from the bloodstream and store it within the muscles. However, it is also important to keep in mind that physical activity will have a different effect on your blood glucose level depending on several different factors, including how long you were physically active, how much energy you expended, exercise intensity, type of exercises performed and much more. Whilst these impact the outcomes, exercise can lower your blood glucose levels for up to 24 hours or more, making your body much more sensitive to insulin after your workout.
The type of exercise you choose is essential when managing type 2 diabetes. A combination of aerobic exercise and strength training is often recommended:
Aerobic Exercise:
Strength Training:
The timing of your exercise can influence its impact on blood sugar levels. To optimise glucose control:
Diabetes can affect the nerves and circulation in your feet, making them more prone to injury. When engaging in physical activity, wear well-fitting, comfortable shoes and examine your feet regularly for blisters, sores, or signs of infection.
Embarking on an exercise routine doesn’t have to be intimidating. Here are some tips to help you get started:
In conclusion, the benefits of exercise for treating type 2 diabetes cannot be overstated. It is a powerful and accessible tool that offers a multitude of advantages for those living with this chronic condition. Regular physical activity can help to:
It is important to remember that, while exercise is a powerful ally in managing health conditions, it should be pursued with care and attention. Consultation with a healthcare provider is crucial to developing a personalised exercise plan that suits your individual needs and capabilities.
Incorporating exercise into your daily routine is not just a strategy for treating type 2 diabetes; it’s a fundamental step toward a healthier, happier life. As with any significant change, the key is consistency. Whether you prefer a brisk walk, a swim, or a session at the gym, the long-term benefits of regular exercise for diabetes management make the effort well worth it. So, take that first step today, and let exercise be your partner in the journey to better health and well-being.
Written by Accredited Exercise Physiologist Kaitlyn Eisenhuth from Activ8 Health Club.
References: https://www.niddk.nih.gov/health-information/diabetes/overview/diet-eating-physical-activity

There is a lot of information and conflicting information out there regarding the current exercise recommendations. Furthermore, these keep changing over the years, which makes it even harder to know. It also depends on many other factors, including medical conditions (such as Cardiovascular Disease, Diabetes, Osteoporosis, Endometriosis, Chronic Pain), age level, gender and even the intensity of exercises undertaken throughout the week. In saying that, we have tried our best to give you the latest information (Current to 2023) regarding the most common situations in the simplest digestible (get it…?) form.
Within the apparently healthy population (a state of complete physical, mental and social well-being and not merely the absence of disease and infirmity as stated by WHO), individuals are unsure if they’re hitting the recommended amount of weekly exercise minutes. Due to this, a greater case in the development of lifelong conditions such as diabetes and heart disease has occurred, leading to a rise in global levels of sickness and death.
Needless to say, exercise is an amazing way to help prevent, manage or delay the onset of these prevalent conditions, along with so many more benefits, but you may be thinking, what exactly should you be doing, and how many minutes you should be aiming for? Well, this blog will uncover all the information you need to know!
Physical inactivity is a term that is not uncommonly used, particularly among Australians. Due to the natural demands of life, such as work, children/family commitments and hobbies, along with other aspects such as injury, individuals may struggle to have the time, motivation or desire to partake in exercise, which is completely understandable! In saying this, it is thought that nearly 60% of Australian adults, and 70% of pregnant women, do not meet the recommended weekly exercise minutes, resulting in an increased likelihood of developing lifelong chronic conditions.
Enough about the negative side of things, though, as you may be thinking about what the benefits of being physically active are. Well, similarly to the negative impacts of physical inactivity, exercise has flow-like effects too! Being physically active has the overarching goal of reducing the likelihood of developing chronic conditions, as mentioned, but there is much more to delve into.
Exercise holds numerous benefits both physically, mentally and even socially! Starting with the mental benefits, exercise is a prime way to release our happy hormones called endorphins. The release of these happy chemicals helps reduce levels of stress and increase feelings of well-being, which in tandem helps reduce levels of depression and anxiety. Furthermore, the physical benefits of exercise come in abundance, primarily reducing the risk of obesity, which reduces or maintains blood pressure, total cholesterol and blood sugar levels. Further improvement in quality of life, sleep quality and energy levels also occurs. This then can be linked to the overarching stem of reducing the likelihood of developing chronic conditions!
There are three (3) main modalities of exercise: cardiovascular, resistance, and flexibility. Each of these modalities holds various and numerous benefits, but they are a fantastic mixture when used in tandem with each other!

As mentioned, the ideal minutes are different between populations, so depicted in the table below are three subgroups associated with the apparently healthy population.
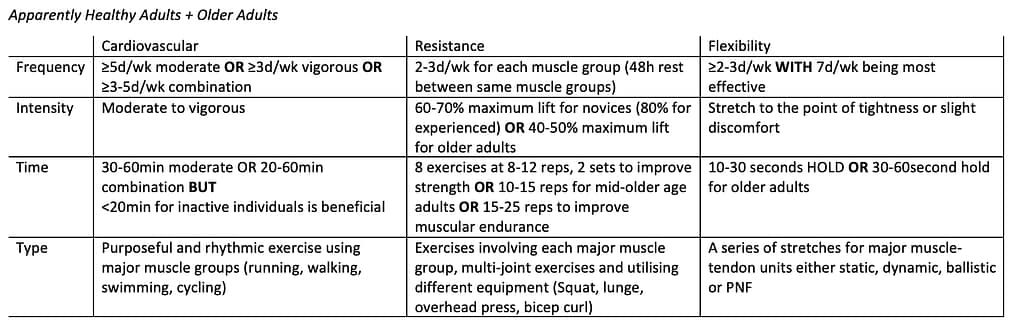
2. Pregnant Women
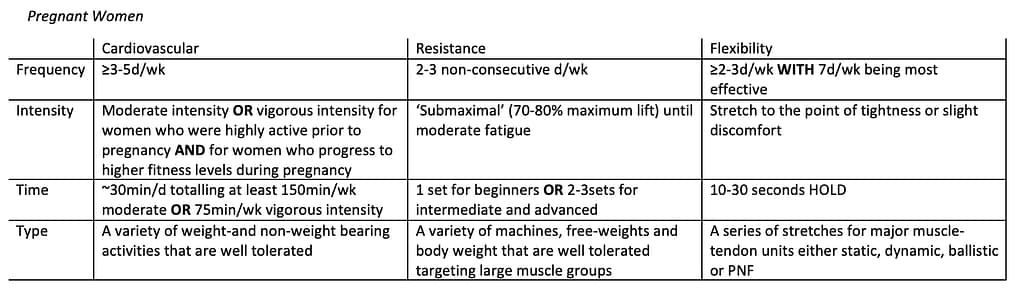
3. Individuals with Lower Back Pain
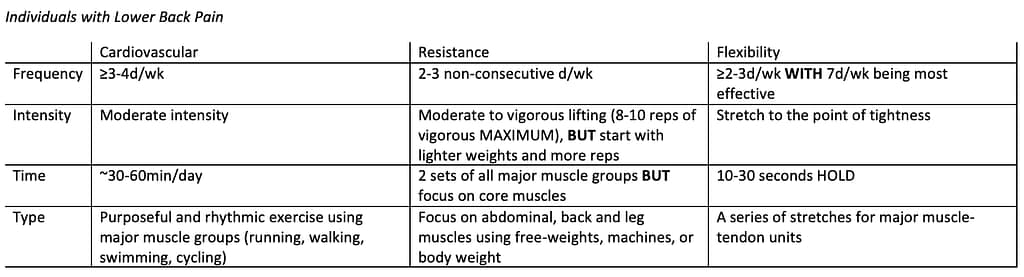

In summary, it’s important to acknowledge that any amount of exercise, no matter how brief, is a step in the right direction toward a healthier lifestyle. However, when we delve deeper into the realm of fitness and well-being, we find that the most significant rewards, both for our physical and mental health, emerge when we commit to a more structured exercise routine.
The magic number to aim for is approximately 150 minutes of weekly cardiovascular exercise, ideally supplemented with resistance and flexibility training. This balance strikes a harmonious chord in our pursuit of overall wellness. Why, you ask?
First and foremost, cardiovascular exercise elevates our heart rate, strengthens our lungs, and enhances circulation, effectively boosting our cardiovascular health. This form of exercise, which includes activities like brisk walking, running, cycling, and swimming, plays a pivotal role in reducing the risk of heart disease, stroke, and hypertension.
On the other hand, resistance training, such as weightlifting or bodyweight exercises, empowers our muscles and bones. This crucial component of the ideal workout routine not only helps sculpt a toned physique but also fortifies our skeletal system. By engaging in resistance training at least a couple of times a week, we can actively combat the decline in muscle mass associated with aging and promote better metabolic health.
Flexibility training, often encompassed by practices like yoga or stretching exercises, enhances our range of motion and helps prevent injuries. It keeps our joints supple and muscles pliable, reducing the risk of strains, sprains, and other physical mishaps.
But perhaps the most compelling reason to strive for this comprehensive exercise regimen is its role in disease, illness, and injury prevention, management, and delay. Regular exercise, when combined with a balanced diet and other healthy lifestyle choices, can be a formidable ally against chronic diseases like diabetes, obesity, and certain types of cancer. It helps manage conditions such as arthritis and osteoporosis, improving overall quality of life. Moreover, it aids in the prevention of injuries by enhancing our physical resilience and reducing the risk of accidents.
In essence, while any minute of exercise is undoubtedly better than none, it’s the dedication to a well-rounded exercise routine that truly unlocks the extensive benefits for our body and mind. It’s a commitment to your health, longevity, and vitality. So, as you embark on your fitness journey, remember that striving for approximately 150 minutes of weekly cardiovascular exercise, complemented by resistance and flexibility training, is a powerful formula that can lead to a healthier, happier you, while simultaneously delaying, managing, or preventing a host of diseases, illnesses, and injuries.
Written by Accredited Exercise Physiologist Paolo Mitry from Activ8 Health Club